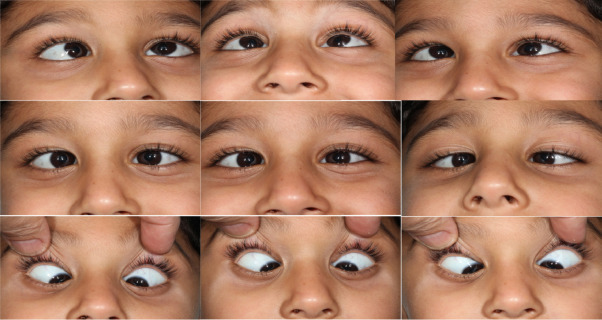
Parents and educators often notice certain eye behaviours in children that raise questions or concerns. One such behaviour is lateral gaze, where a child looks at objects, people, or surroundings from the side of their eyes rather than directly.
While this behaviour can appear unusual or even concerning, lateral gaze is not always a problem. Understanding what lateral gaze is, why it occurs, and when it needs attention helps caregivers respond appropriately and support the child effectively.
What Is Lateral Gaze?
Lateral gaze refers to a pattern in which a child frequently looks sideways, using their peripheral vision instead of looking straight ahead. The child may turn their head away while still keeping the object within their field of view.
This behaviour is commonly observed in some children with:
- Autism Spectrum Disorder (ASD)
- Sensory processing differences
- Visual–motor integration challenges
Importantly, lateral gaze is not simply a habit or naughty behaviour. It is often a neurological or sensory strategy that the child uses to process visual information more comfortably.
Why Do Children Use Lateral Gaze?
Children may use lateral gaze for several underlying reasons related to how their brain processes sensory and visual input.
1. Sensory Processing Differences
Some children find direct visual input overwhelming. Using peripheral vision helps reduce sensory overload and allows them to engage with their environment more comfortably.
2. Visual–Motor Integration Challenges
Difficulties in coordinating eye movements with head and body movements may lead children to rely on sideways viewing instead of direct gaze.
3. Primitive Reflex Retention
Retained primitive reflexes such as ATNR (Asymmetrical Tonic Neck Reflex) or TLR (Tonic Labyrinthine Reflex) can interfere with:
- Midline control
- Eye–head coordination
- Smooth visual tracking
This can contribute to lateral gaze patterns.
4. Neurological Differences
In children with autism, lateral gaze may be a way to:
- Self-regulate
- Maintain focus
- Interpret visual information differently
5. Avoidance of Social Demand
Direct eye contact can feel intense or uncomfortable for some children. Looking sideways allows them to participate socially without emotional overload.
When Is Lateral Gaze a Concern?
Occasional sideways looking is developmentally normal. However, lateral gaze becomes clinically relevant when it:
- Interferes with learning or attention
- Affects social interaction
- Impacts reading, writing, or copying tasks
- Occurs frequently along with poor postural control
- Is associated with delayed developmental milestones
Persistent or repetitive lateral gaze requires further observation and professional assessment.
Assessment of Lateral Gaze in Occupational Therapy
An occupational therapist evaluates lateral gaze through a comprehensive and child-friendly assessment process. This includes examining:
- Eye tracking and visual scanning skills
- Midline crossing abilities
- Postural stability
- Bilateral coordination
- Sensory processing patterns
- Primitive reflex integration
- Visual–motor integration
Standardised assessment tools, clinical observation, and play-based evaluation help identify the root cause of lateral gaze and guide intervention planning.
Occupational Therapy Intervention Strategies
Occupational therapy focuses on addressing the underlying sensory, motor, and visual challenges contributing to lateral gaze.
1. Sensory Regulation Activities
These activities help organise the nervous system and include:
- Deep pressure input
- Proprioceptive activities such as pushing, pulling, and climbing
- Vestibular input like swinging or gentle rocking
2. Visual–Motor Activities
To strengthen eye control and tracking:
- Tracking games using bubbles or flashlights
- Visual scanning worksheets
- Ball games that encourage midline focus
3. Postural Control and Core Strengthening
Strong postural stability supports better eye alignment and control. Activities include:
- Prone play activities
- Therapy ball exercises
- Animal walks
Together, these strategies improve visual engagement, attention, and functional participation.
Supporting the Child at Home and School
Parents and educators play a key role in supporting children with lateral gaze.
Helpful strategies include:
- Avoid forcing eye contact
- Allow gradual and comfortable visual engagement
- Follow the child’s sensory needs
- Encourage play that naturally promotes looking and tracking
- Work closely with therapists and educators
Creating a supportive environment helps the child feel safe while developing stronger visual and sensory skills.
Who Should Be Aware of Lateral Gaze?
1. Parents and Caregivers
Parents are often the first to notice lateral gaze. Understanding that it is not misbehaviour but a coping strategy enables better support at home.
2. Children with Developmental Differences
Lateral gaze may be seen in children with:
- Autism Spectrum Disorder (ASD)
- Sensory processing difficulties
- Visual–motor integration challenges
- Developmental delays
- Retained primitive reflexes
3. Occupational Therapists
OTs assess underlying sensory, motor, and visual factors and plan appropriate intervention strategies.
4. Teachers and Special Educators
Educators benefit from understanding lateral gaze to:
- Reduce visual overload
- Adapt classroom environments
- Support learning without forcing eye contact
5. Early Intervention Professionals
Speech therapists, physiotherapists, psychologists, and early intervention specialists work collaboratively to support overall development and participation.
Key Takeaway
Lateral gaze is communication, not misbehaviour.
It reflects how a child’s brain processes sensory and visual information.
With proper understanding, assessment, and occupational therapy support, children can develop:
- Improved visual engagement
- Better attention
- Enhanced functional participation
Early identification and intervention play a vital role in helping children feel comfortable, confident, and capable in their daily environments.
Dr. Deepa
senior occupational therapist